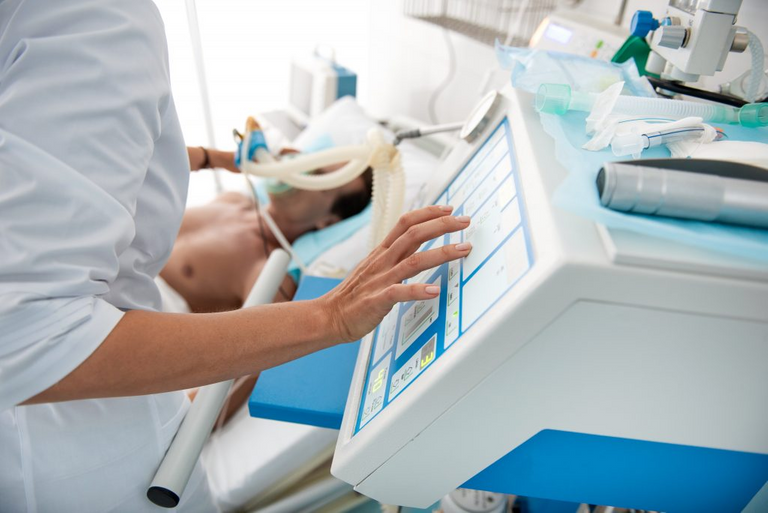
I have seen many people discussing mechanical ventilators and the role they are playing in the treatment of COVID-19. Many have speculated that they may be overused.
I'd like to give a little bit of background about what a mechanical ventilator is and why it is used, and then offer my perspective as it stands based on what I currently know based on my own research and from talking with friends and other experts on the front-line treating COVID patients.
What is a mechanical ventilator:
It is a machine designed to be attached to a tube inserted in the trachea to take over the lung function of someone who is no longer able to breathe. It has a variety of modes and settings, but when a person's lungs fail, the ventilator is designed to keep them alive while their lungs have a chance to recover. As you can imagine, a ventilator is not a benign contraption, and it is possible to cause a variety of injuries to the lungs with the ventilator.
Here's the dilemma with which clinicians are currently faced:
COVID-19 patients are known to decompensate rapidly and often unexpectedly. That is, a rapid deterioration of a previously functioning system in their body (like heart function, kidney function etc.) You see, if they are on a ventilator, and their respiratory status worsens, then one can change the ventilator settings in an effort to correct this. However, if they are not on a ventilator, this is a dire emergency.
It is especially a dire emergency because connecting a human being to a ventilator is not simple, easy or low-risk. The procedure, known as intubation, usually goes something like this:
Pre-oxygenate the patient as much as possible, so that they have as much oxygen in their blood as you can get (not easy in someone decompensating from COVID-19).
Administer an anethetic drug to put the patient to sleep.
(Usually) administer a paralytic drug to make it so they cannot move any of their muscles....at this point, the patient can not longer breathe at all on their own, and the clock starts ticking. You can administer oxygen by ambu-bag, but in a patient with serious lung disease you may not have the ability to administer enough, and many of the ways you can do this create aerosolized particles (risking potential airborne transmission).
Use a device called a laryngoscope, which resembles a large metal blade, to move the jaw and the tongue out of the way and get a clear view of the trachea and vocal cords.
Insert the tube into the trachea, inflate the balloon on the tube, and then go through a series of checks to make sure the tube is actually in the trachea.
If this makes you nervous, well, it should. Of the doctors, nurses, respiratory therapists and everyone involved, all have expressed how nervous this makes them too. What if their anatomy is not standard and you can't see their trachea? What if you have trouble actually inserting the tube? These things happen, and they can lead to the patient's death.
Now, if you are intubating someone for surgery, who has normal lungs, or if you are intubating them for high carbon dioxide, it is lower risk, because you have more time and if something goes wrong you can troubleshoot. But if you are intubating them for hypoxia, you are really in the highest risk situation.
There's another wrinkle here: for COVID-19 patients, the procedure itself aerosolizes the virus--so you really want to make sure when you do this, that you're doing it under optimal conditions, every item you need laid out it in its appropriate position, video equipment ready and working, the most qualified person available to do the intubation, etc.
If you are intubating a COVID-19 patient, you don't want to be making multiple attempts in a shit show of an intubation, you want it to go smoothly, for your safety and the patient's safety. The best way to make an intubation go smoothly is to prepare in a deliberate fashion, not rush to the bedside as someone's heart starts to slow down.
So, here you are with COVID-19 patients, with low oxygen saturations, who are known to decompensate very quickly, and you're learning that some of these people can pull through without ventilators.
If you put someone on a ventilator, but they could/would have pulled through without it, you've done them a disservice. But if you wait too long to put them on a ventilator, the risk that they die while you are doing it, or die before you have a chance to do it, goes up.
How to balance these risks?
How do you avoid intubating those who don't need to be intubated, while also ensuring maximum safety?
In an ideal world, you would have a way to know who is going to recover without a ventilator and who isn't. You really don't know, unfortunately. Maybe with time this can be figured out.
You could put these people in negative pressure rooms (those are in shorter supply than ventilators), put them on advanced non-invasive oxygen, and watch them closely--which is what some people are starting to do (reportedly what PM Boris Johnson received.)
This is far more resource intensive than just intubating them. This is probably the ideal situation. Yes, you can prone them to increase their oxygenation ability--but the idea of having someone off a ventilator when the difference for them between life and death is laying on their stomach, is pretty scary.
So how do you navigate this, given resource constraints, given the need to protect staff, given the unknowns and the potential for very rapid deterioration and the high risks that presents to the patients?
Well, it turns out that people are trying to figure that out. Little by little, people are getting better at this.
I want to make something clear, though: while mortality is very high for patients on ventilators with COVID-19, I do not think that is directly caused by the ventilators themselves. The mortality would certainly be even higher without the ventilators.
The salient question at the moment is how far to push things prior to intubation. There are differing views on this, I think I've laid out the basic view here, which is that if you are to avoid early intubation it is by careful planning of a safety system to do crash intubations well, putting these patients in ICU even though they aren't on ventilators, and watching them like hawks.
This ties into the final point: Reducing ventilator use is only possible in very resource-rich environments, with lots of staff, negative pressure rooms, PPE etc available.
People can't snap our fingers and make those resources appear, but people can practice social distancing, to make sure that hospitals can give this kind of very, very detailed and resource-intensive attention to each patient.
One of the doctors I spoke to said that they feel comfortable delaying some intubations precisely because their hospital isn't overwhelmed, and therefore can keep a good eye on the patients.
Social distancing is key to keeping this level of care possible.
